So, you thought life after hysterectomy would be life without your original problem – fibroids, endometriosis, painful periods, etc. But now other problems are springing up: anxiety, fatigue, low libido, hot flashes, etc. Life’s never fair! And that’s why, in this post, we’re going to consider hormone therapy after hysterectomy.
Regardless of the reasons you had a hysterectomy, or the type of surgery you had, one thing is sure: You can still live a healthy and vibrant life after hysterectomy with the help of bioidentical hormone replacement therapy (BHRT).
To help you understand the impact of a hysterectomy on your hormone levels and the options you have for managing the symptoms of early menopause and other health problems, we’ve gathered everything you need to know in this post.
We want you to be able to make an informed decision about choosing BHRT as a potential solution for restoring your hormonal balance and improving your overall wellbeing after surgery.
Different Types of Hysterectomy
How Hysterectomy Affects Your Hormones
Other Considerations About Hormone Therapy After Hysterectomy
Hormone Therapy Can Benefit Your Recovery Post Hysterectomy
BHRT: the Recommended Hormone Therapy After Hysterectomy
More Ways to Support Your Overall Health After a Hysterectomy
Understanding Hysterectomy: What It Is and Why You Might Need It
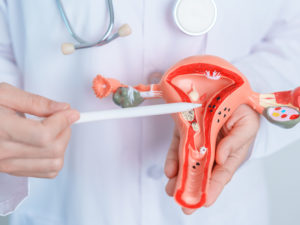 Hysterectomy is a surgical procedure that involves removing a woman’s uterus and (often) some of its surrounding organs (see below). Doctors usually recommend it for different medical conditions, including the following:
Hysterectomy is a surgical procedure that involves removing a woman’s uterus and (often) some of its surrounding organs (see below). Doctors usually recommend it for different medical conditions, including the following:
- Uterine fibroids
- Uterine cancer
- Ovarian cancer
- To treat severe endometriosis
- Uterine prolapse
- Adenomyosis
- Chronic pelvic pain
- Abnormal or heavy menstrual bleeding
Depending on the severity of your condition, your doctor may recommend other treatments before performing a hysterectomy.
For example, if you have uterine fibroids, they could advise a uterine fibroid embolization instead of surgery. But if your doctor realizes uterine fibroid embolization may not solve your issue, they’ll likely recommend a hysterectomy.
There are different kinds of hysterectomy involving total or partial removal of the female reproductive organs. Your healthcare provider will decide which one you should have, depending on the condition you need treating.
Different Types of Hysterectomy
 A total hysterectomy removes your entire uterus, including your cervix – the lower part of the uterus that connects to the vagina. This may be recommended for treating large uterine fibroids, for example.
A total hysterectomy removes your entire uterus, including your cervix – the lower part of the uterus that connects to the vagina. This may be recommended for treating large uterine fibroids, for example.
A partial hysterectomy involves the removal of the upper part of your uterus while leaving the cervix intact. This procedure is usually chosen when your cervix is healthy, and there’s no specific reason to remove it.
Finally, a radical hysterectomy is the removal of your uterus, cervix, the surrounding tissues, and possibly the upper part of your vagina. This procedure is typically performed for gynecological cancers, such as cervical or endometrial cancer, or when the disease has spread to nearby structures. If you also have ovaries removed, it’s called oophorectomy.
How Hysterectomy Affects Your Hormones
Having your uterus and other sexual organs removed can affect your hormonal dynamics and many body functions, particularly if you had your ovaries removed. This is because they’re the primary source of estrogen, progesterone, and testosterone production in premenopausal women.
If your hysterectomy is partial, your hormonal levels may be affected to some extent, but the impact is typically less significant compared to a total or radical hysterectomy with one or both ovaries removed, which will cause you to experience surgical menopause.
Surgical menopause describes the sudden decline or interruption in the production of hormones vital for your reproductive cycle and overall wellbeing. And sadly, surgical menopause is unavoidable if you have your ovaries removed.
In natural (peri)menopause, this decline is gradual and may last up to 10 years until you finally reach menopause. But with a hysterectomy, these abrupt hormonal changes can result in sudden early menopause symptoms that your body was not yet prepared to experience if you’re not of menopausal age.
So – these early menopause symptoms may include (but are not limited to) the following:
- Severe hot flashes
- Night sweats
- Mood swings
- Vaginal dryness
- Fatigue
- Low libido
- Anxiety
- Insomnia
- Depression
Other Considerations About Hormone Therapy After Hysterectomy
Due to the disruption of the hormonal balance in your body and the sudden lack of estrogen caused by surgical menopause, you should also consider some long-term, hormone-based health issues after hysterectomy – because they can directly influence your bones and heart health.
- Bone thinning: Estrogen plays a crucial role in maintaining bone density and preventing bone thinning. Its deficiency after a hysterectomy may increase the risk of osteoporosis and fractures. In addition to a healthy lifestyle and a balanced diet with vitamin D supplements, hormone therapy slows bone thinning.
- Cardiovascular health: Estrogen protects the cardiovascular system and limits your risk of stroke. Its decline may increase your risk of heart disease.
Hysterectomy is an invasive procedure that may significantly impact your quality of life if you don’t address symptoms like hot flashes, vaginal dryness, or low sex drive. That’s a given. But in addition to the physical impact, surgical menopause can also affect your mental and emotional health.
For many women, post-hysterectomy challenges are not limited to hormonal fluctuations and estrogen deficiency.
There’s a psychological and emotional impact of losing your reproductive organs and the natural ability to conceive. That’s why it’s crucial to have mental and medical support if you undergo surgical menopause.
Make sure you talk to your healthcare provider, as well, if you’re facing any of the following challenges and symptoms on top of hormone imbalance and early menopause symptoms:
- Long-lasting pain, heavy bleeding, and abdominal cramps. These are considered normal for a few days or weeks after the surgery, but if they persist for longer, you should talk to your doctor.
- Insomnia, mood swings, sense of loss, and depression. After removal of your reproductive organs, it’s common to experience a sense of loss or grief, even when you don’t want to give birth to children. Please get emotional and psychological support if this is you.
- Body image concerns. Changes in the physical appearance or function of your reproductive organs may affect body image and self-esteem. Talk to your healthcare provider to help you commit to lifestyle choices that will help you recover your confidence.
Living with all the changes after your hysterectomy can be difficult, but you don’t need to do it alone. Your healthcare provider is there for guidance, support, and potential hormone therapy options – such as BHRT – to help manage your symptoms and promote your overall wellbeing.
Hormone Therapy Can Benefit Your Recovery Post Hysterectomy

You now know why it’s impossible to think of hysterectomy without considering its impact on your hormone levels!
In fact, most of the menopause symptoms and challenges you’re facing are due to the hormonal rollercoaster you’ve been riding after the surgery.
For this reason, hormone therapy after hysterectomy is a sensible choice. It can play a significant role in helping you recover and manage symptoms – reestablishing your hormonal balance by replacing the hormones that your body no longer produces due to surgical menopause.
However, traditional hormone replacement therapy uses standard dosages of synthetic hormones.
This one-size-fits-all approach doesn’t necessarily work for everyone because it hasn’t necessarily taken into account your body’s specific needs.
It’s important you have the correct type and dose of hormone therapy after hysterectomy.
Let’s say you need estrogen only. Or, perhaps your doctor may recommend a combination of estrogen and progesterone to minimize the impact of too much estrogen in your body – which could increase the risk of breast cancer and ovarian cancer if you use it long term.
BUT you also need a specific dose of either of these hormones after your healthcare provider has assessed your unique hormone deficiency.
In addition, like any medication, traditional hormone therapy may cause some uncomfortable side effects, including the following:
- Nausea
- Headaches
- Changes in weight
- Diarrhea
- Low libido
- Anxiety
Side effects vary from person to person. They’re also influenced by the type of hormone therapy you’re taking – maybe estrogen alone (the purported dangers of estrogen-only therapy were debunked years ago) or a combination of estrogen and progesterone, as we said.
To minimize the side effects and improve efficacy, Nava Health recommends a customized approach to hormone replacement therapy using bioidentical hormone replacement therapy (BHRT).
Keep reading to discover why BHRT is the best option for post-hysterectomy women dealing with the challenges of surgical menopause.
BHRT: the Recommended Hormone Therapy After Hysterectomy
BHRT refers to using hormones structurally identical to the hormones your body naturally produces. Because they have the same chemical structure as your hormones, there are fewer risks of side effects but increased tolerance of the treatment.
Unlike the synthetic forms used in traditional HRT (see above), these bioidentical hormones are
- derived from natural sources, such as yam or soy, and
- prepared by compounding pharmacies to create custom-made hormone formulations in various dosage and forms, including creams, gels, capsules, or pellets.
BHRT uses natural estrogen, progesterone, and sometimes testosterone to supplement or replace the hormones that may be deficient or imbalanced in your body and effectively treat the symptoms you’re experiencing after a hysterectomy.
The main advantage of using BHRT instead of traditional HRT is its personalized nature – BRHT can be custom-made and tailored to meet your body’s specific hormone needs.
Your healthcare provider oversees the administration of your custom-made BRHT and provides you with the correct dosage and amount of hormones. Your doctor will also do regular checkups to ensure ongoing appropriate dosage and evaluate your treatment’s effectiveness and safety.
Benefits of BHRT as Your Hormone Therapy After Hysterectomy
When used for treating early menopause symptoms after a hysterectomy, BHRT and estrogen therapy are particularly beneficial for:
Improving Bone Health and Preventing Bone Thinning
Estrogen deficiency after your hysterectomy can lead to
- accelerated bone loss,
- early bone thinning, and
- an increased risk of osteoporosis.
Estrogen replacement therapy can help compensate for the decline in your estrogen levels, helping to maintain a more optimal hormonal environment for bone health, slowing bone thinning, reducing the risk of fractures, and helping preserve bone density. Vitamin D supplements are also essential to prevent bone thinning.
Relieving Menopause Symptoms
Estrogen replacement therapy can also help relieve common menopause symptoms – such as hot flashes, night sweats, mood swings, and vaginal dryness that may occur after a hysterectomy – by restoring hormonal balance.
Supporting Cardiovascular Health
Estrogen also has cardio-protective effects, helping to maintain healthy blood vessels and reducing the risk of heart disease. Hormone replacement and estrogen therapy can help mitigate those potential cardiovascular risks associated with declining estrogen levels after your hysterectomy.
More Ways to Support Your Overall Health in Addition to Hormone Therapy After a Hysterectomy
In addition to BHRT, you can commit to healthy lifestyle habits to help restore hormone balance and address your post-hysterectomy menopausal symptoms.
The following activities will support your overall health and wellbeing post hysterectomy.
An Estrogen-Rich Diet
Eating foods rich in phytoestrogens is beneficial for maintaining healthy estrogen levels. You can also increase your consumption of fiber, iron, vitamin supplements E and D, and calcium, in addition to your estrogen therapy. This helps prevent early bone thinning.
The following foods also help regulate your hormone levels:
- Broccoli
- Cabbage
- Soy
- Brussel sprouts
- Flax seeds
- Garlic
- Peas
- Beans
- Legumes
Physical Activities
Regular exercise will help prevent weight gain, promote good health, and restore hormonal balance after your hysterectomy.
Also consider pelvic floor strengthening activities. Hysterectomy may impact your pelvic floor muscles, especially if surgery involved removing your cervix. Engaging in pelvic floor exercises like Kegels can help strengthen these muscles and support urinary and bowel control.
Enough Sleep
We know it’s difficult to sleep well with hot flashes. But sleep deprivation can contribute to
- mood disturbances,
- increased levels of stress,
- hormone imbalance, and
- reduced mental clarity.
So, try to have at least 6-8 hours of quality sleep every night! Good sleep supports your mental and emotional wellbeing, helping you maintain a positive mindset, cope with stress, and better manage any emotional challenges that may arise during recovery.
It’s one more reason to consider having hormone replacement therapy after your hysterectomy.
 The Importance of Hormone Replacement Therapy After Hysterectomy: Nava Can Help
The Importance of Hormone Replacement Therapy After Hysterectomy: Nava Can Help
If you want to learn more about estrogen therapy or the other forms of hormone therapy after your hysterectomy – and how they can help in your post-hysterectomy recovery from hormone imbalance – Nava practitioners can help you consider BHRT.
Hysterectomy is disruptive, there’s no doubt about it. You cannot avoid an early menopause. And the sudden appearance of menopausal symptoms like mood swings or hot flashes can impact all areas of your life. But with the help of an empathetic healthcare provider specializing in BHRT, you will get your life back!
Our practitioners at Nava Health specialize in integrative medicine, taking the time to listen to you, assess your health and hormonal levels, and create a comprehensive, customized treatment plan that addresses your symptoms and specific hormonal needs.
Make an appointment with us today to learn more about hormone therapy after hysterectomy and how we can help improve your quality of life.